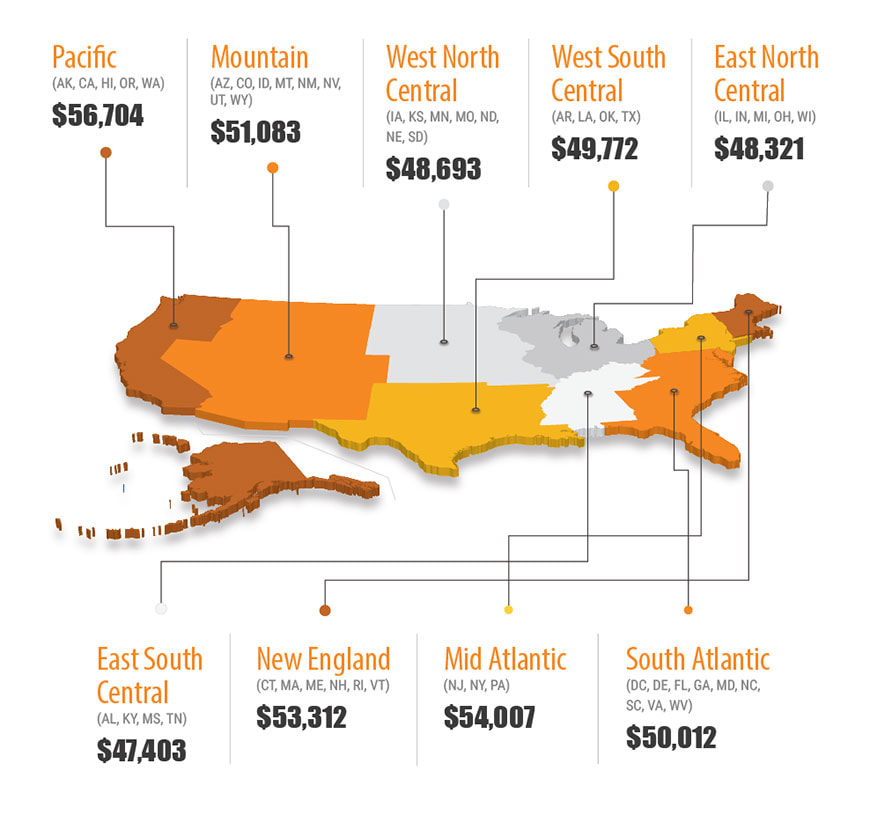
What is medical coding?Medical coding and medical billing are typically referred to so interchangeably that many people have come to be under the impression that the two are the same thing. Quite on the contrary, there are distinct and important differences between the two terms that need to be understood thoroughly by those looking to enter the field. A large part of the reason for this confusion is undoubtedly that the two separate functions are often performed by individuals who work in very close proximity to one another. In fact, According to the American Academy of Professional Coders, both of these procedures are actually frequently encompassed in one position. Medical billers use given codes to indicate to payment agencies, insurance companies and clearing houses which procedures have been performed for a patient by their practice. In order to schedule these billings, billers rely on coders to provide them with accurate informational codes representing any and all combinations that a given practice could have provided. Where do medical coders work?1. Hospitals & doctor’s offices There’s no surprise here! Hospitals need medical coders to document and assign codes for each medical procedure a patient receives. They research codes, interpret patient charts and use specialized medical coding software to assign the proper codes. Doctor’s offices and specialty clinics, such as dermatology or dental offices, also use medical coders to process billing and insurance claims. Hospital patients may receive a number of treatments from several different physicians. That means hospital medical coders should be prepared for plenty of critical thinking and research to track down obscure medical codes. This can be a fun challenge, but don’t rule out working in a smaller, specialty clinic. “Specialties pay more,” Reid says. “There is always an opportunity to grow your knowledge and expand your coding credentials depending on your interests.” 2. Insurance agencies Medical coders who work for insurance agencies see patient claims from the other side of the table. They verify the accuracy of incoming claims and note if any information is missing or incorrect. Then they compare the treatment a patient received to their insurance plan coverage so payments can be processed. Medical coders who work in the insurance industry will need to have a solid understanding of medical codes and be willing to do the research to fill in the gaps. An eye for detail is critical since catching errors is one of their main job duties. They should also be up for the challenge of interpreting the details of insurance plans. 3. Information technology or service management companies Many IT companies develop software and products to help healthcare facilities streamline their medical coding and billing processes. Some technical companies even offer services, such as auditing, to catch any errors or incorrect procedures in a clinic or hospital. Medical coders play a vital role in these companies. They’re responsible for conducting audits and reviews to ensure accurate coding and prevent rejected claims due to coding errors. Some medical coders may even teach a class to show healthcare employees how to avert coding errors in the future. 4. Educational institutions Colleges and technical schools need experienced medical coders to train the next generation of coding students. There are no official educational requirements for medical coders, but the BLS states there are certifications that can be earned from an accredited institution. These schools offer plenty of opportunities for trained medical coders to share their knowledge with students. Teaching jobs typically require a few years of on-the-job experience, so they make a great option for seasoned medical coders who are ready for a change of pace. This is the perfect career path for anyone who loves the ins and outs of medical coding and enjoys sharing their wisdom with others. 5. Law firms Billing fraud is a big problem for healthcare providers. Incorrect billing procedures can cause a provider to come under fire for fraud—even if it was unintentional. A provider has to prove that any billing and coding errors were simply mistakes, or they may face criminal charges. Law firms often hire medical coders to help investigate fraud claims. These coders will examine records to help determine if coding mistakes were intentional or the result of billing fraud. A thorough knowledge of Medicaid laws and regulations is a necessity in this medical coding position. 6. Government agencies State and federal government agencies, such as the National Center for Health Statistics or state Medicaid departments, are another employer of medical coders. These daily job duties are similar to those of medical coders in other industries: assigning codes, abstracting information and reviewing and auditing incoming claims codes. Government agencies offer the opportunity to work on projects that may affect healthcare across the nation. Plus there’s another big benefit: the federal government offers some of the highest medical coding salaries in the field, according to a study by the American Association of Professional Coders (AAPC). 7. Your living room That’s right, you could be a successful medical coder from the comfort of your own home—or anywhere else you have reliable Internet access! There are plenty of legitimate work-from-home coding jobs available; just make sure to be on the lookout for scammers. You could even start your own medical coding business like Beth Morgan, president of Medical Detectives, did. “Being my own boss allows me freedom and flexibility, and I am able to assist all sources of providers,” Morgan says. She enjoys the unique opportunity she has to perform coding reviews for companies and agencies spanning all of the industries described above. If you prefer variety and could picture yourself working in any of these settings, the self-employed route may be the perfect solution for you! *This information was found at: www.rasmussen.edu/degrees/health-sciences/blog/where-do-medical-coders-work/ What is the average salary of a certified medical coder?*Salary image from the American Academy of Professional Coders website, July 2017. What is the job security of a medical coder?The 2012-2013 edition of the Occupational Outlook Handbook, published by the U.S. Department of Labor, estimates:
How do I become a medical coder?Earning a bachelor’s degree or master’s degree can strengthen a medical coder's career; however, it's not required to show proficiency. What is necessary is to have a solid foundation of anatomy, physiology, and medical terminology education, which can be obtained by earning the Certified Professional Coder credential. It's recommended for serious coders to complete a medical coding course of study and pass an exam to designate him or her as a CPC®. Employers know CPCs® are individuals who can perform medical coding tasks with the utmost proficiency and excellence. Here at Amundsen Educational Center, our Professional Medical Coding Program teaches you what you need to know in order to become a Certified Professional Coder. Our small class size and knowledgeable staff provide you with all of the tools you will need to be successful. Helpful Links to more Information
18 Comments
2/28/2018 10:45:23 pm
Good Post.
Reply
7/23/2019 06:42:09 am
It's good to know that medical coders send information about what procedures were performed on a patient to insurance companies for billing purposes. My daughter wants to enter the healthcare field, but she doesn't want to deal with blood and needles. I'll pass this information along to her so that she can look further into her options for becoming a medical coder.
Reply
10/4/2019 10:36:14 am
I like that you said that having a strong solid foundation on physiology and medical terminology education can help you become a coder. I have a friend that said that she wants to study hard to get a good spot in the medical industry. I'm going to share this information with her so that she knows what to study.
Reply
10/15/2019 02:38:32 pm
Thanks for the information on medical coding! My cousin wants to set up a healthcare clinic. He would probably need help with medical coding.
Reply
7/24/2020 05:59:57 am
I like what you said about medical coding services being in high demand. My sister wants to make sure that her medical bills are done properly in the coming weeks. I'll share this information with her so that she can look into her options for professionals who can help her with this.
Reply
6/17/2021 03:58:47 am
Hey thanx for sharing this blog over here. It seems useful to start career in clinical research. We will look forward for more updates.
Reply
10/26/2021 10:00:53 pm
Hi There! Thanks for sharing this amazing resource material. You have done a great job on emphasizing the career and scope in medical coding. Will definitely visit this site again to read more intrusive content like these!!
Reply
10/26/2021 10:59:45 pm
Great Content!! I found this article to be very helpful and informative especially because you have described and stressed quite well about the future of medical coding.
Reply
11/2/2021 07:28:27 am
Thanks for Sharing medical coding service article. <a href="https://www.billingmd360.com/medical-coding-services-in-usa.html">Medical Coding Service in the USA
Reply
1/12/2022 04:45:55 am
I never knew that medical coding and medical billing are typically referred to so interchangeably that many people have come to be under the impression that the two are the same thing. I never thought that it would be like this, it is a good article to read, I'll share this with my aunt. Thank you for the information about medical coding.
Reply
1/15/2022 09:00:46 am
Hi, great blog post that completely explains all the futuristic options related to the Medical coding
Reply
2/24/2022 12:10:34 am
This is a very purposeful and useful information one should have. The in formation provided above can be seen in only some articles like this. I personally thank the article writer for writing such knowledgeable information with all of us. thank you.
Reply
12/15/2023 11:41:54 pm
I can't thank you enough for your medical coding blog. Your straightforward approach has made learning coding much more enjoyable. Your efforts in simplifying the content are truly appreciated
Reply
12/27/2023 03:17:10 am
Thanks for writing about medical coding in such a simple way. I understood everything without any trouble
Reply
2/5/2024 12:01:33 am
A very detailed information on medical coding and its average pay scale i appriciate it
Reply
This blog post highlights the expanding opportunities in medical coding, emphasizing its pivotal role across various sectors like hospitals, insurance agencies, IT firms, educational institutions, law firms, government agencies, and even remote work setups. As medical coders play a crucial role in healthcare operations, ensuring accuracy and compliance with coding standards is essential. If you're considering a career in medical coding or seeking reliable coding services, understanding these diverse employment avenues and the demand for skilled coders can guide your decisions effectively.
Reply
Leave a Reply. |
AuthorBridgit Gillis Archives
October 2017
Categories
All
|
Location |
|

 RSS Feed
RSS Feed

